Page 1

Loading page ...
Page 2
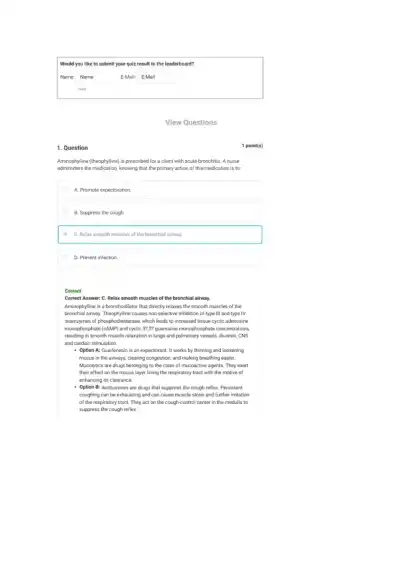
Loading page ...
Page 3
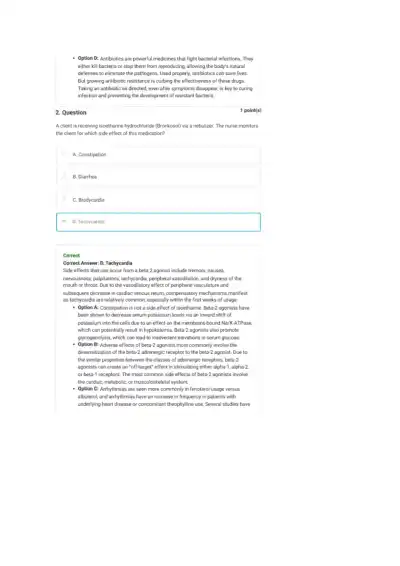
Loading page ...
Page 4
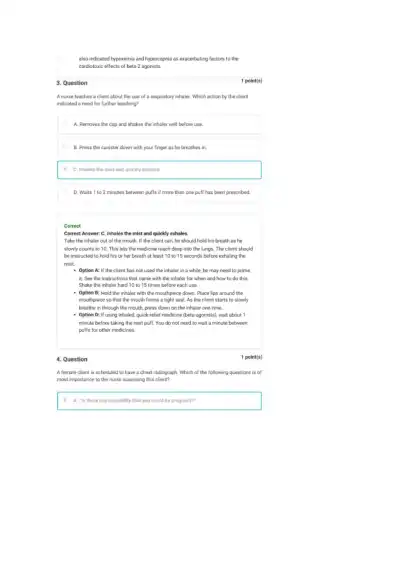
Loading page ...
Page 5
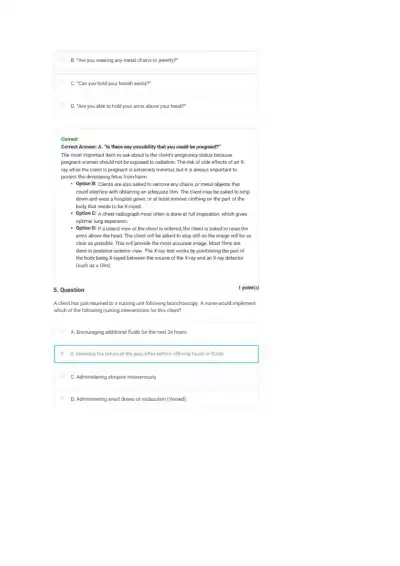
Loading page ...
Page 6

Loading page ...
Page 7
Loading page ...
Page 8
Loading page ...
Page 9

Loading page ...
Page 10

Loading page ...
Page 11

Loading page ...
Page 12
Loading page ...
Page 13
Loading page ...
Page 14

Loading page ...
Page 15

Loading page ...
Page 16

Loading page ...
Page 17
Loading page ...
Page 18

Loading page ...
Page 19
Loading page ...
Page 20

Loading page ...
Page 21
Loading page ...
Page 22
Loading page ...
Page 23
Loading page ...
Page 24
Loading page ...
Page 25

Loading page ...
Page 26

Loading page ...
Page 27

Loading page ...
Page 28

Loading page ...
Page 29

Loading page ...
Page 30
Loading page ...
Page 31
Loading page ...
Page 32
Loading page ...
Page 33
Loading page ...
Page 34
Loading page ...
Page 35

Loading page ...
Page 36
Loading page ...
Page 37

Loading page ...
Page 38

Loading page ...
Page 39

Loading page ...
Page 40
Loading page ...
Page 41
Loading page ...
Page 42
Loading page ...
Page 43
Loading page ...
Page 44
Loading page ...
Page 45
Loading page ...
Page 46
Loading page ...
Page 47

Loading page ...
Page 48
Loading page ...
Page 49
Loading page ...
Page 50
Loading page ...
Page 51

Loading page ...
Page 52

Loading page ...
Page 53
Loading page ...
Page 54
Loading page ...