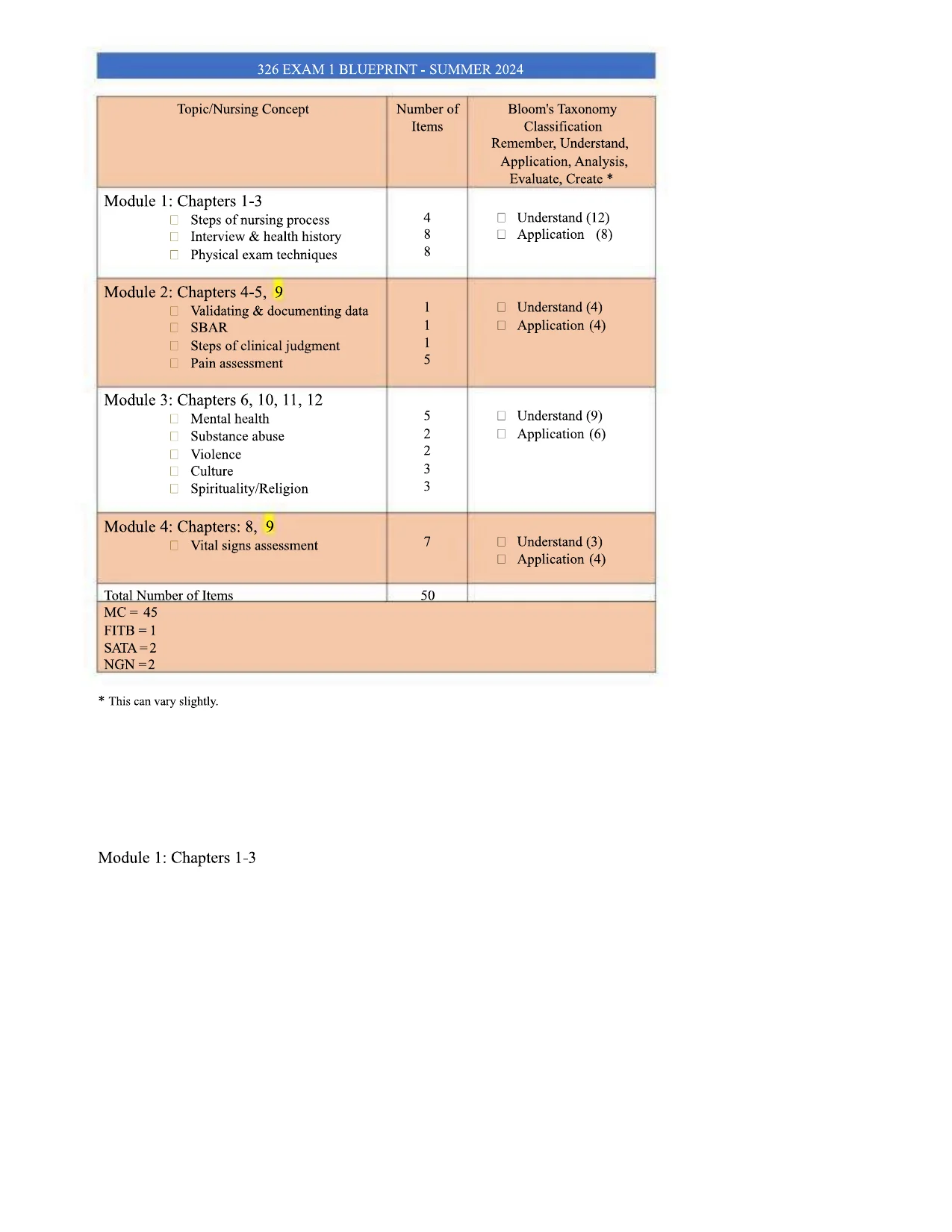
326 EXAM 1 BLUEPRINT - SUMMER 2024Topic/Nursing ConceptNumber ofItemsBloom's TaxonomyClassificationRemember, Understand,Application, Analysis,Evaluate, Create *Module 1: Chapters 1-3□Steps of nursing process□Interview & health history□Physical exam techniques488□Understand (12)UApplication(8)Module 2: Chapters 4-5, 9nValidating & documenting data□SBARSteps of clinical judgmentHPain assessment1115□Understand (4)□Application (4)Module 3: Chapters 6, 10, 11, 12HMental health□Substance abuse□Violence□Culture□Spirituality/Religion52233UUnderstand (9)□Application (6)Module 4: Chapters: 8, 9□Vital signs assessment7□Understand (3)□Application (4)Total Number of Items50MC= 45FITB = 1SATA= 2NGN =2* This can vary slightly.Module 1: Chapters 1-3
326 EXAM 1 BLUEPRINT - SUMMER 2024Topic/Nursing ConceptNumber ofItemsBloom's TaxonomyClassificationRemember, Understand,Application, Analysis,Evaluate, Create *Module 1: Chapters 1-3□Steps of nursing process□Interview & health history□Physical exam techniques488□Understand (12)UApplication(8)Module 2: Chapters 4-5, 9nValidating & documenting data□SBARSteps of clinical judgmentHPain assessment1115□Understand (4)□Application (4)Module 3: Chapters 6, 10, 11, 12HMental health□Substance abuse□Violence□Culture□Spirituality/Religion52233UUnderstand (9)□Application (6)Module 4: Chapters: 8, 9□Vital signs assessment7□Understand (3)□Application (4)Total Number of Items50MC= 45FITB = 1SATA= 2NGN =2* This can vary slightly.Module 1: Chapters 1-3Preview Mode
This document has 17 pages. Sign in to access the full document!